Content Menu
● What is Procaine HCL Injection?
● Preparing for Administration
● Step-by-Step Administration Procedure
● Dosage Guidelines and Safety Precautions
>> Management
● Storage and Handling of Procaine HCL Injection
● FAQ
>> 1. What is the maximum dose of Procaine HCL Injection?
>> 2. How should Procaine HCL Injection be diluted for infiltration anesthesia?
>> 3. Who should avoid Procaine HCL Injection?
>> 4. What are common side effects of Procaine HCL Injection?
>> 5. Can Procaine HCL Injection be administered at home?
Procaine Hydrochloride (HCL) Injection is a widely utilized local anesthetic in medical and dental procedures to provide temporary numbness or loss of sensation in specific areas. It belongs to the ester-type local anesthetic class and works by blocking nerve impulse conduction in peripheral nerves. Its typical applications include surgeries, dental treatment, and minor invasive procedures where localized anesthesia without sedation is required. Proper administration of Procaine HCL Injection is essential to achieve effective anesthesia, limit systemic toxicity, and avoid adverse reactions. This comprehensive guide covers patient assessment, dosage calculation, injection techniques, precautions, side effects, storage, and frequently asked questions to support healthcare professionals in safely managing Procaine HCL Injection.
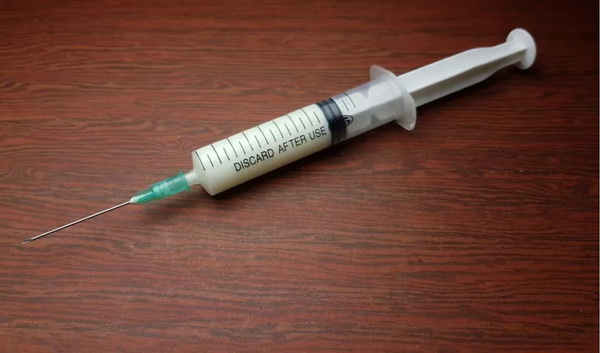
Procaine HCL Injection is a sterile injectable solution of procaine hydrochloride generally available in 1%, 2%, or 10% concentrations. It is primarily indicated for local infiltration anesthesia, peripheral nerve blocks, and neuraxial anesthesia such as spinal or epidural blocks. Upon injection, procaine temporarily blocks sodium channels in nerve membranes, stopping the generation and conduction of nerve impulses, which results in numbness or loss of pain sensation. Procaine is known for its relatively short onset (2-5 minutes) and moderate duration (20-40 minutes), making it suitable for procedures that require rapid onset and recovery.
Before the administration of Procaine HCL Injection, a thorough clinical evaluation is critical. This includes obtaining a detailed medical history, with emphasis on allergies (especially to ester-type anesthetics), cardiac, hepatic, and renal status, and concurrent medications that could interact or potentiate anesthetic effects. Special caution is required for elderly or debilitated patients and those with compromised organ function, as dose adjustments may be necessary because of altered metabolism and clearance of procaine.
The dosing of Procaine HCL depends on the procedure, site, patient weight, and clinical condition. For adults, the maximum single dose should generally not exceed 1000 mg per treatment session to avoid systemic toxicity. Typical doses for infiltration anesthesia range from 350 to 600 mg, with concentrations between 0.25% and 0.5%. Pediatric doses vary but can be up to 15 mg/kg for infiltration anesthesia.
Procaine HCL Injection comes predominantly in 1% and 2% sterile aqueous solutions. For infiltration anesthesia, these solutions are often diluted to lower concentrations (0.25%-0.5%) by adding sterile isotonic sodium chloride (0.9%) saline. Vasoconstrictors like epinephrine may be added in concentrations of 1:100,000 to 1:200,000 to reduce systemic absorption, prolong anesthetic effect, and control bleeding.
Procaine HCL Injection can be administered using various routes depending on the type and extent of anesthesia needed:
- Subcutaneous Injection: For local infiltration anesthesia, procaine is injected slowly into the subcutaneous tissue surrounding the surgical or procedural site.
- Intramuscular Injection: Administered into large muscle groups for regional anesthesia over a wider area.
- Peripheral Nerve Block: Injection near specific peripheral nerves provides anesthesia to targeted limbs or regions, helpful for orthopedic or dental procedures.
- Neuraxial Anesthesia: Intrathecal or epidural injections of a 10% procaine solution provide anesthesia and muscle relaxation to larger body segments for surgeries or labor.
Each route requires strict aseptic technique and precise anatomical knowledge to avoid complications such as intravascular injection or nerve injury.
1. Equipment Preparation:
- Use sterile gloves, syringes, and needles appropriate for the route. Verify the Procaine HCL Injection vial or ampoule for expiration and clarity.
2. Patient Positioning:
- Position the patient suitably according to injection type: lateral decubitus or sitting for spinal anesthesia, relaxed supine or prone for peripheral blocks.
3. Site Preparation:
- Disinfect the skin at the injection site using an antiseptic solution with a circular motion moving outward to reduce infection risk.
4. Injection Technique:
- Aspirate before injecting to ensure the needle is not within a blood vessel.
- For infiltration, inject slowly and uniformly around the site.
- For nerve blocks, advance the needle carefully to the nerve vicinity using anatomical landmarks or ultrasound guidance. Inject procaine incrementally with frequent aspiration.
- For neuraxial routes, inject slowly at about 1 mL every 5 seconds, observing patient tolerance.
5. Monitoring:
- Continuously monitor the patient for adverse reactions such as allergic symptoms, CNS toxicity, or cardiovascular effects. Vital signs should be checked before, during, and after administration.
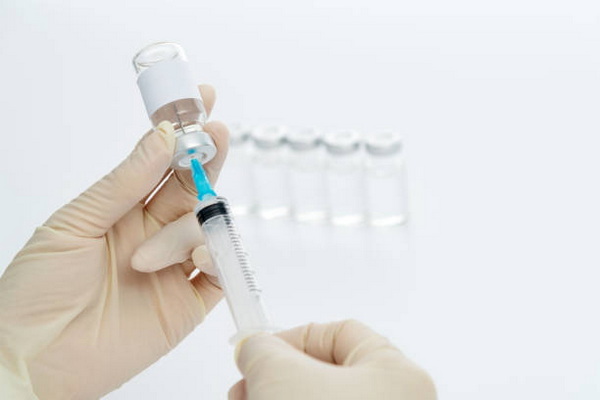
- The maximum dose of Procaine HCL should not exceed 1000 mg per single treatment session for adults.
- For infiltration, dilution to 0.25% or 0.5% is standard; prepare by mixing one part of the 1% solution with an appropriate volume of sterile 0.9% saline (e.g., 30 mL 1% procaine + 30 mL saline for a 0.5% solution).
- Epinephrine addition is optional depending on the procedural context but recommended for vasoconstriction and prolonged anesthesia effect.
- Dose adjustments are recommended for elderly patients and those with renal, hepatic, or cardiac impairment to prevent accumulation and toxicity.
- Rapid injection or large-volume injections should be avoided to prevent systemic toxicity and high circulating levels.
- Avoid use in patients with known hypersensitivity to ester anesthetics or those with methemoglobinemia.
- Mild local reactions such as redness, swelling, or pain at the injection site.
- Dizziness, lightheadedness, or drowsiness following systemic absorption.
- Allergic reactions including rash, urticaria, or anaphylaxis requiring immediate intervention.
- Central nervous system toxicity presenting as confusion, seizures, or respiratory depression.
- Cardiovascular issues such as hypotension, arrhythmias, or cardiac arrest in cases of overdose.
- Immediately discontinue injection if symptoms of toxicity or allergy appear.
- Supportive care including oxygen administration, seizure control, and cardiovascular support is crucial in severe cases.
- Administer epinephrine promptly in anaphylactic reactions.
Proper storage and handling ensure product efficacy and patient safety:
- Store Procaine HCL Injection at controlled room temperature (15-30°C), protected from light and moisture.
- Maintain aseptic techniques during preparation and administration to avoid contamination.
- Keep out of reach of unauthorized personnel and children.
The safe and effective administration of Procaine HCL Injection plays a vital role in providing local and regional anesthesia for various medical procedures. Comprehensive patient assessment, precise dosage calculation, and meticulous injection technique are essential to maximize anesthetic benefits while minimizing the risk of adverse events. By adhering to established guidelines and safety precautions, healthcare professionals can confidently use Procaine HCL Injection to manage procedural pain effectively. For pharmacies, clinics, and hospitals seeking high-quality Procaine HCL Injection or OEM pharmaceutical manufacturing, partnering with experienced and reliable suppliers is key to ensuring consistent product quality and patient safety.
If you require premium Procaine HCL Injection products or professional OEM manufacturing services tailored for international markets, contact us at SupplyBenzocaine.co.uk. Our factory specializes in secure, high-standard production with complete compliance to global regulations. Connect with our experts today to discuss your specific needs and receive a customized quote.
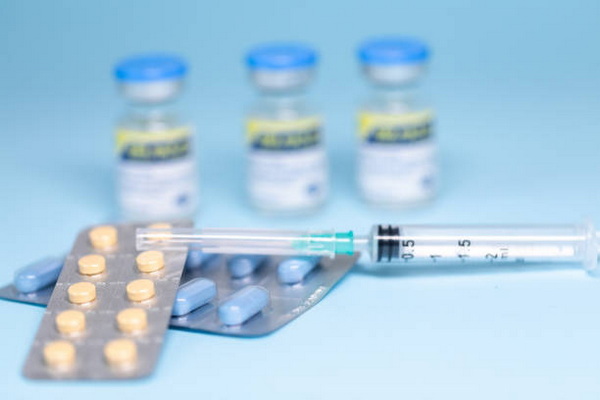
The advised maximum dose for adults is 1000 mg per session, adjusted by weight and patient health status. Doses exceeding this increase the risk of systemic toxicity.
For a 0.5% dilution, mix 30 mL of 1% Procaine with 30 mL of sterile 0.9% sodium chloride solution. For 0.25%, mix 15 mL of 1% solution with 45 mL of saline.
Patients allergic to ester-type local anesthetics, those with severe liver, kidney, or heart disease without dose adjustment, and those with methemoglobinemia should avoid or consult healthcare professionals before use.
Common side effects include mild injection site redness, swelling, dizziness, or drowsiness. Severe reactions like allergic responses or CNS toxicity require prompt medical attention.
No. Due to potential complications including allergic reactions and toxicity, Procaine HCL Injection must be administered only by trained healthcare professionals in clinical settings.
[1](https://www.ncbi.nlm.nih.gov/books/NBK551556/)
[2](https://drugs.ncats.io/drug/95URV01IDQ)
[3](https://dailymed.nlm.nih.gov/dailymed/fda/fdaDrugXsl.cfm?setid=c80c810a-60e0-49bd-139c-95aec3a286fc)
[4](https://magistralbr.caldic.com/storage/product-files/1590302101.pdf)
[5](https://go.drugbank.com/drugs/DB00721)
[6](https://archive.hshsl.umaryland.edu/bitstreams/3e9f4861-60dd-4d5a-aafd-117ca3d61273/download)
[7](https://www.britannica.com/science/procaine-hydrochloride)
[8](https://jpdb.nihs.go.jp/jp14e/14data/Part-I/Procaine_Hydrochloride.pdf)
[9](https://associationofanaesthetists-publications.onlinelibrary.wiley.com/doi/pdf/10.1111/j.1365-2044.1949.tb05806.x)
[10](https://www.mhlw.go.jp/content/11120000/000945683.pdf)
Hot tags: Procaine Injection Technique, Administering Procaine, Local Anesthetic Administration, Procaine HCL Guidelines, Injection Safety, Medical Procedures, Procaine Dosage, Injection Protocol, Anesthetic Techniques, Healthcare Training