Content Menu
● Procaine: A Historical Overview
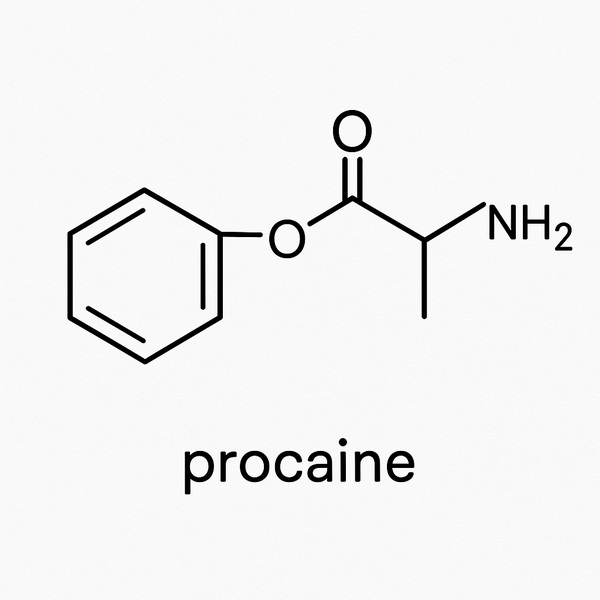
● Chemical Structure and Properties of Procaine
>> Combination with Other Drugs
>> Experimental and Alternative Medicine
● Non-Medical and Alternative Uses
>> Gerovital H3 and the Anti-Aging Movement
● Side Effects and Safety Profile
>> Contraindications and Precautions
● Procaine vs. Other Local Anesthetics
● Research and Future Directions
● FAQ: Top 5 Questions About Procaine
>> 1. What is procaine used for today?
>> 2. Is procaine the same as Novocain?
>> 3. What are the main side effects of procaine?
>> 4. Why is procaine less common today?
>> 5. Can procaine help with aging or cognitive problems?
Procaine is a synthetic compound widely recognized for its central role as a local anesthetic, most notably under the brand name Novocain. Since its discovery in the early 20th century, procaine has influenced modern anesthesia, dentistry, and even areas outside conventional medicine due to its purported rejuvenating effects.
In this extensive article, we will cover procaine's history, chemistry, mechanism of action, medical and non-medical uses, side effects, safety considerations, and more. Through detailed discussions, you will gain a comprehensive understanding of what procaine is and why it remains relevant in biomedical sciences and pharmacology.

Procaine was first synthesized in 1905 by the German chemist Alfred Einhorn, who named it "Novocain," a term combining the Latin "nov-" (“new”) and "-caine," a common suffix for anesthetics. It was introduced into medical practice shortly thereafter by surgeon Heinrich Braun.
Before procaine's invention, cocaine was the predominant local anesthetic, prized for its potent numbing effects but burdened by significant addiction potential and toxicity risks. The arrival of procaine marked a breakthrough by offering a compound that was less toxic, non-addictive, and effective at blocking nerve pain. Procaine's popularity skyrocketed in dentistry and minor surgery, becoming the mainstay anesthetic agent for decades. However, as the 20th century progressed, procaine was gradually replaced by newer anesthetics like lidocaine, which provided a better safety and allergy profile.
Still, procaine's significant contribution to medicine earned it a place in the annals of pharmaceutical history and inspired ongoing research into related ester local anesthetics and their therapeutic potentials.
Procaine is classified as an amino ester local anesthetic. Its molecular formula is C₁₃H₂₀N₂O₂, and it is chemically named 2-diethylaminoethyl p-aminobenzoate. In its pure form, procaine presents as a small, white crystalline powder. For medical use, it is most commonly supplied as procaine hydrochloride, a water-soluble salt that allows for easy formulation into injectable solutions.
- Chemical Formula: C₁₃H₂₀N₂O₂
- Molecular Weight: 236.3 g/mol
- Melting Point: 61°C–63°C (base form)
- Solubility: Water-soluble as hydrochloride salt
- Pharmacological Class: Local anesthetic (ester type)
Unlike amide anesthetics, ester anesthetics like procaine are metabolized rapidly by plasma esterases, which limits their systemic toxicity but also contributes to their relatively short duration of action.
Procaine exerts its anesthetic effect by blocking voltage-gated sodium channels on neuronal cell membranes. These channels are critical for the initiation and propagation of action potentials in nerve fibers. By inhibiting sodium influx through these channels, procaine effectively prevents the generation and transmission of nerve impulses, resulting in localized numbness or loss of sensation.
The specificity of procaine for sensory neurons allows it to produce local anesthesia without depressing consciousness or affecting motor control when administered properly. This property is particularly useful for targeted procedures where pain relief is necessary without systemic effects.
Metabolically, procaine is quickly hydrolyzed in the plasma by pseudocholinesterase enzymes into para-aminobenzoic acid (PABA) and diethylaminoethanol. The rapid degradation helps in the quick cessation of anesthetic action but also introduces PABA, a compound associated with allergic reactions in sensitive individuals.
Procaine is primarily used as a local anesthetic for minor surgical and dental procedures. It is injected directly into tissues or administered near peripheral nerves to block pain sensation in a specific region. Its use is common in areas including but not limited to:
- Dental procedures such as tooth extractions and cavity fillings
- Minor surgical interventions like biopsies or small excisions
- Peripheral nerve blocks for regional anesthesia
- Spinal anesthesia in some settings
- Diminishing pain associated with intramuscular injections, notably penicillin G
Despite its slower onset and shorter duration compared to newer anesthetics like lidocaine, procaine remains valuable in clinical scenarios where these properties are sufficient and cost-effectiveness is prioritized.
Historically, procaine has been combined with antibiotics such as penicillin G to reduce the pain of intramuscular injections. The anesthetic effect smooths the injection experience, thereby improving patient compliance. Some formulations also included epinephrine to prolong anesthesia and minimize bleeding by vasoconstriction, though this practice is less common today due to risk considerations.
Beyond anesthesia, procaine has been explored in alternative medicine and experimental therapies. Since the mid-20th century, it has been investigated for potential benefits such as:
- Anti-aging effects, notably in the formulation known as Gerovital H3
- Cognitive enhancement in elderly patients
- Relief of symptoms associated with chronic diseases, including arthritis and atherosclerosis
- Alleviation of mild depression
However, these purported non-anesthetic benefits remain contentious due to limited scientific evidence supporting their efficacy. As a result, use in these contexts is generally not endorsed by mainstream medical authorities.
Gerovital H3, a proprietary injectible formulation containing procaine and other ingredients, gained fame in the 1950s and beyond for claims of rejuvenation, vitality enhancement, and memory improvement. Developed by Romanian physician Ana Aslan, Gerovital was adopted in various countries and attracted endorsements by celebrities and political leaders.
Despite its popularity, rigorous clinical trials were unable to conclusively validate the anti-aging claims. Regulatory agencies have since emphasized caution, warning patients against unproven off-label use of procaine for aging or chronic disease management without proper medical oversight.
Procaine's physical resemblance to cocaine has unfortunately led to its illegal use as an adulterant in street drugs. Unscrupulous dealers may mix procaine with cocaine to increase volume or mimic cocaine's appearance, which poses significant health risks due to unknown purity and effects.
This illicit usage is dangerous and illegal, highlighting the importance of controlled pharmaceutical production and distribution.
When used properly by healthcare professionals, procaine's safety profile is generally favorable. Common mild side effects are usually localized and transient, including:
- Localized numbness and tingling around the injection site
- Minor pain, swelling, or bruising at the site of administration
These effects typically resolve quickly without intervention.
Though rare, more severe reactions can occur and should be promptly recognized:
- Allergic responses ranging from mild skin rash to anaphylaxis
- Cardiovascular effects such as bradycardia (slow heartbeat), hypotension, or arrhythmias
- Central nervous system symptoms including dizziness, drowsiness, excitement, tremors, or seizures
- Systemic lupus erythematosus-like symptoms potentially triggered by prolonged or oral exposure to procaine
Proper patient history taking and allergy testing may help mitigate the risk of allergic reactions.
Procaine administration should be avoided or used cautiously in:
- Individuals with known hypersensitivity to ester-type local anesthetics or related compounds
- Patients with pseudocholinesterase enzyme deficiency, which slows metabolism and increases toxicity risk
- Those with a history of systemic autoimmune conditions such as lupus
Pregnant and breastfeeding women require careful evaluation before procaine use due to insufficient safety data in these populations.

The development of anesthetics has evolved significantly, giving rise to newer compounds like lidocaine, an amide local anesthetic, which has largely supplanted ester anesthetics like procaine.
| Feature | Procaine | Lidocaine |
|---|---|---|
| Chemical Type | Ester | Amide |
| Onset of Action | Slow | Rapid |
| Duration | Short | Medium to long |
| Allergy Risk | Higher (due to PABA release) | Lower |
| Current Usage | Limited, mostly historical | Widely used in diverse clinical settings |
Lidocaine's faster onset, longer duration, and lower allergy incidence make it preferable for most modern clinical applications. Nevertheless, procaine's historical importance and continued niche utility remain recognized.
Dentistry was one of the first fields to widely adopt procaine after its discovery. The compound provided a revolutionary alternative to cocaine, offering pain relief without addiction risks or severe systemic toxicity. Its introduction transformed dental practice by enabling reliable and relatively safe local anesthesia.
Dentists appreciated procaine's benefits, and it became the standard anesthetic for many decades. Although modern dentists now favor amide anesthetics like lidocaine due to improved efficacy and safety, procaine's pioneering role in dental anesthesia is undisputed.
While procaine's use as a local anesthetic is decreasing, research persists in exploring its possible ancillary effects and derivatives. There is ongoing scientific interest in formulations like Gerovital H3 and their potential neurologic or geriatric applications.
Additionally, procaine's chemical structure and mechanism serve as templates for designing new anesthetic agents or drug delivery systems targeting specific tissues with minimal side effects.
Further investigation may clarify the scope of procaine's therapeutic possibilities beyond conventional anesthesia, although rigorous clinical trials are essential to validate such potential.
Procaine represents a landmark discovery in the history of anesthesia. Once the gold standard for pain control in minor surgery and dentistry, its role has diminished with the advent of newer anesthetics offering superior efficacy and safety. Yet, its contribution to medical science remains invaluable, having paved the way for safer local anesthesia practices.
While procaine is generally safe when used appropriately, awareness of its risks, contraindications, and potential allergic reactions is crucial. Alternative uses in anti-aging or neurological contexts remain scientifically controversial and lack robust evidence.
In contemporary medicine, procaine's practical applications are limited, but ongoing research continues to explore its broader physiological effects and potential new uses. For patients and clinicians alike, understanding procaine's properties and history enriches the appreciation of anesthetic pharmacology's evolution.
Procaine is currently used mainly as a local anesthetic for minor surgical and dental procedures. It also serves as an agent to reduce pain during intramuscular antibiotic injections. Alternative uses such as anti-aging treatments exist but are not supported by strong scientific evidence.
Yes, Novocain is a brand name for procaine. The terms are often used interchangeably. "Novocaine" is a common variant spelling, particularly in the United States.
Common side effects include numbness, tingling, or minor pain at the injection site. Severe reactions, such as allergic responses or neurological symptoms like seizures, are rare but possible, especially with high doses or in susceptible individuals.
Procaine has been largely replaced by anesthetics like lidocaine, which offer faster onset, longer duration, and fewer allergic reactions. Improved safety profiles and broader versatility have made lidocaine the preferred choice in most cases.
Though procaine has been promoted in alternative medicine, particularly through preparations like Gerovital H3, scientific studies have not conclusively supported its effectiveness for anti-aging or cognitive enhancement. Its use for these purposes is not widely endorsed by medical professionals.
Hot tags: What Is Procaine Used For, Procaine Definition And Uses, Medical Uses Of Procaine, Procaine Local Anesthetic, Procaine Benefits And Side Effects, Procaine Vs Lidocaine, How Procaine Works, What Is Procaine Hydrochloride, Procaine Injection Uses, Procaine For Pain Relief