Content Menu
● 1. What Are Procaine and Morphine?
>> Procaine: A Local Anesthetic Agent
>> Morphine: The Opioid Analgesic
● 2. Chemical and Pharmacological Comparison of Procaine and Morphine
● 3. Clinical Applications and Therapeutic Use
>> Procaine in Clinical Practice
>> Morphine in Clinical Practice
>> Combined Use and Synergistic Effects
● 4. Safety Considerations and Side Effects
● 5. Research and Future Directions
● FAQ
>> 1. What is the primary difference between procaine and morphine?
>> 2. Can procaine and morphine be used together safely?
>> 3. What are the main side effects of morphine?
>> 4. How is procaine metabolized in the body?
>> 5. Is there any chemical relationship between procaine and morphine?
Procaine and morphine are two well-known substances used widely in the medical field for pain management and anesthesia. While both drugs target pain control, they belong to different drug classes and exert their effects through distinct mechanisms of action. Understanding the relationship between procaine and morphine, including their pharmacology, clinical uses, and interactions, is essential for healthcare providers, pharmaceutical manufacturers, and OEM service providers in the biotechnology, medical device, and pharmaceutical industries.
This comprehensive article explores the scientific and clinical connections between procaine and morphine, covering their chemical structures, mechanisms, clinical applications, similarities, differences, and potential combined use. The discussion further scrutinizes their interactions in pain management and highlights ongoing research. Finally, the article includes an informative FAQ section to address common queries and concludes with a call to action for interested professional partners.
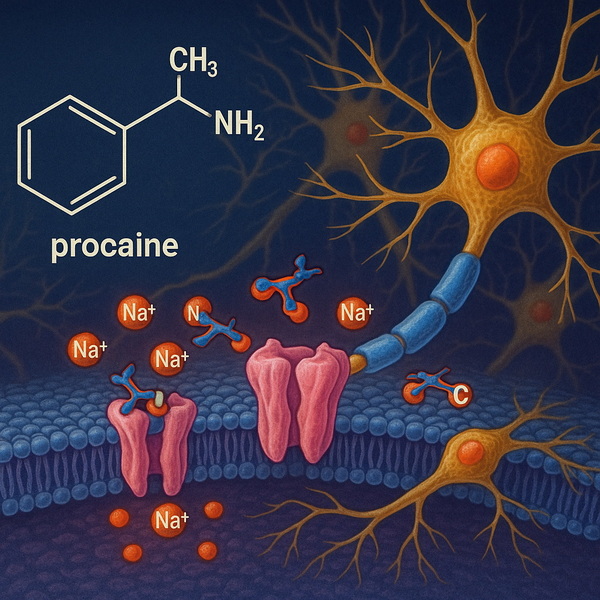
Procaine is an ester-type local anesthetic widely used to induce temporary regional or local numbness. Developed in the early 20th century, it remains a fundamental drug in dental treatments, minor surgical procedures, and other local anesthesia applications.
- Chemical class: Ester local anesthetic
- Primary use: Local and regional anesthesia
- Mechanism of action: Procaine works by blocking voltage-gated sodium channels on the neuronal membranes, which halts the influx of sodium ions necessary for generating nerve impulses. This blockage prevents the transmission of pain signals from the site of administration to the brain.
- Pharmacokinetics: Procaine is rapidly hydrolyzed by plasma esterases into para-aminobenzoic acid (PABA), which is then excreted renally.
- Duration: Procaine has a relatively short duration of action, with an approximate plasma half-life of 6 to 10 minutes.
- Clinical considerations: It can cause local irritation and allergic reactions in sensitive individuals due to the PABA metabolite.
Morphine, derived from the opium poppy, is a powerful opioid pain reliever commonly used for moderate to severe pain relief in acute and chronic settings.
- Chemical class: Opioid alkaloid agonist
- Primary use: Systemic pain management
- Mechanism of action: Morphine binds to opioid receptors (primarily mu-opioid receptors) located in the brain and spinal cord. By activating these receptors, morphine inhibits the release of neurotransmitters involved in pain signaling and alters the perception and emotional response to pain.
- Pharmacokinetics: It undergoes hepatic metabolism primarily via glucuronidation to active metabolites like morphine-6-glucuronide, which also have analgesic effects.
- Duration: Morphine's analgesic effect onset ranges from 5 to 30 minutes, with variable duration depending on administration route.
- Clinical considerations: Morphine use carries significant risks, including respiratory depression, tolerance development, dependence, and potential for addiction.
Although both procaine and morphine are essential in pain management, they differ fundamentally in their chemical structures, mechanisms, and clinical roles.
- Chemical Structure: Procaine is an ester-based local anesthetic, whereas morphine is an opioid alkaloid with a complex phenanthrene ring structure.
- Mechanism: Procaine induces local numbness by inhibiting sodium channels in peripheral nerves, blocking nerve impulse propagation. Morphine acts centrally, binding opioid receptors to modulate pain perception.
- Pharmacodynamics: Morphine provides systemic pain relief affecting CNS centers responsible not just for nociceptive signals but also emotional pain processing, unlike procaine's localized peripheral effect.
- Administration: Procaine is typically administered via local infiltration or regional blocks around surgical sites or dental nerves. Morphine can be administered orally, intravenously, intramuscularly, subcutaneously, epidurally, or intrathecally.
- Metabolism and Duration: Procaine has rapid metabolism with a short duration, requiring administration close to the target site and time of procedure. Morphine's longer duration allows for sustained pain control systemically.
Despite these differences, both drugs have complementary roles in varying clinical scenarios, often used in combination protocols to optimize patient comfort and pain control.
Procaine's primary application is in creating local anesthesia during surgical procedures such as dental extractions, minor skin surgeries, and blockade of small nerve branches. Its rapid onset and short duration make it ideal for outpatient or brief interventions. Additionally, procaine has been explored for anti-inflammatory effects and some neuromodulatory applications, although these uses are less common.
Morphine remains a cornerstone opioid analgesic for managing moderate to severe pain in hospital, palliative, and pain clinic settings. It is used in post-operative pain management, cancer pain, trauma, and severe chronic conditions like advanced arthritis or neuropathic pain syndromes. Morphine's potent analgesic effect, central activity, and well-characterized pharmacology make it indispensable but also require careful monitoring for side effects and dependency.
Though chemically different, procaine and morphine can be used in combination or sequentially to provide multimodal pain management:
- Local anesthetics like procaine can numb the surgical site while morphine provides systemic analgesia to prevent or reduce pain perception and emotional distress.
- Some clinical studies suggest local anesthetics may potentiate the analgesic effects of morphine, allowing for lower opioid doses and reduced side effects.
- In regional anesthesia techniques such as epidurals or nerve blocks, morphine may be administered alongside local anesthetics including procaine derivatives to extend analgesia duration and improve postoperative pain control.
- Reports also show reduced opioid consumption and enhanced patient satisfaction when local anesthetics and opioids are combined.
This multimodal approach targets different pain pathways, synergistically improving analgesic efficacy and minimizing adverse drug effects.
Procaine is generally safe when administered correctly but can cause:
- Local allergic reactions due to PABA metabolite
- Local irritation or tissue damage if injected improperly
- Systemic toxicity is rare due to rapid metabolism but can occur with overdose
Morphine's well-known risks include:
- Respiratory depression, potentially fatal at overdose levels
- Development of tolerance and physical dependence with prolonged use
- Constipation, nausea, sedation, and other opioid-related adverse effects
- Risk of addiction and abuse, requiring careful medical supervision
Understanding these side effect profiles is critical for pharmaceutical production and OEM providers supplying these drugs, especially when designing combination products or delivery devices to maximize safety and efficacy.
The interaction between procaine and morphine continues to be a subject of pharmacological research:
- Studies are investigating molecular mechanisms behind the synergistic analgesic effects observed in combination therapies.
- There is interest in developing new formulations combining local anesthetics and opioids for improved postoperative pain protocols.
- Research also explores safer, non-addictive opioid alternatives potentiated by local anesthetics or other adjuncts.
- Innovations in delivery systems such as liposomal formulations aim to control release profiles enhancing the duration and minimizing toxicities.
For companies engaged in biomedical manufacturing and OEM services, these advances represent valuable opportunities for product innovation and clinical application enhancement.
In summary, procaine and morphine, while not chemically related, are intimately connected through their complementary roles in pain management. Procaine, a local anesthetic, works by blocking nerve conduction locally, providing temporary numbness, whereas morphine, an opioid analgesic, acts systemically on central opioid receptors to modulate pain perception and responses.
Their combined use in clinical settings demonstrates the benefits of multimodal analgesia, potentially enhancing pain relief while minimizing individual drug side effects. For biotechnology, pharmaceutical, and medical device manufacturers, understanding these drugs' distinct characteristics and interaction potential is essential for developing effective, safe, and innovative products.
If you are interested in OEM service collaboration regarding procaine, morphine, or related medical and pharmaceutical products, or seek advanced biotechnological solutions integrated with medical devices, we invite you to contact us for professional consultation and partnership opportunities.
Procaine is a local anesthetic that blocks nerve signal transmission by inhibiting sodium channels, causing localized numbness. Morphine is an opioid analgesic that binds to opioid receptors in the central nervous system to relieve pain system-wide.
Yes, they can be used together and often are, especially in surgical and pain management settings, to provide both localized anesthesia and systemic pain relief with improved efficacy.
Morphine can cause respiratory depression, tolerance, physical dependence, constipation, sedation, and has significant addiction potential requiring careful medical oversight.
Procaine is rapidly hydrolyzed by plasma esterases into para-aminobenzoic acid (PABA), which is then eliminated primarily through the kidneys.
No, procaine is an ester local anesthetic, while morphine is an opioid alkaloid. They have distinct chemical structures and mechanisms of action.
[1] https://go.drugbank.com/drugs/DB00721
[2] https://go.drugbank.com/drugs/DB00295
[3] https://www.ahajournals.org/doi/pdf/10.1161/01.CIR.5.4.551
[4] https://pubmed.ncbi.nlm.nih.gov/19535707/
[5] https://www.sciencedirect.com/science/article/pii/0014299968901611
[6] https://www.sciencedirect.com/science/article/pii/S0022356525057672
[7] https://link.springer.com/article/10.1007/BF03015229
[8] https://pubmed.ncbi.nlm.nih.gov/1854026/
[9] https://www.cancer.gov/research/participate/clinical-trials-search/v?id=NCI-2022-00035
Hot tags: Procaine, Morphine, Pain Management, Local Anesthetics, Opioid Analgesics, Drug Interactions, Anesthesia, Pharmacology, Pain Relief Medications, Anesthetic Agents