Content Menu
● How Procaine Works: Pharmacology and Mechanism of Action
● Procaine as a Vasodilator: Detailed Mechanisms
● Clinical Implications of Procaine-Induced Vasodilation
● Balancing Vasodilation and Anesthetic Duration
● Frequently Asked Questions (FAQ)
>> 1. What is procaine mainly used for?
>> 2. How does procaine cause vasodilation?
>> 3. Why is procaine administered with a vasoconstrictor?
>> 4. Can procaine cause low blood pressure?
>> 5. Is procaine safer than other local anesthetics?
Procaine, belonging to the amino ester local anesthetic group, is a widely utilized agent for producing localized anesthesia in medical and dental procedures. Besides its common use for pain relief, procaine exhibits significant pharmacological properties that include vasodilation—the widening of blood vessels—that affects blood flow and tissue perfusion. This article explores the detailed mechanisms by which procaine acts as a vasodilator, its clinical significance, safety profile, and applications.
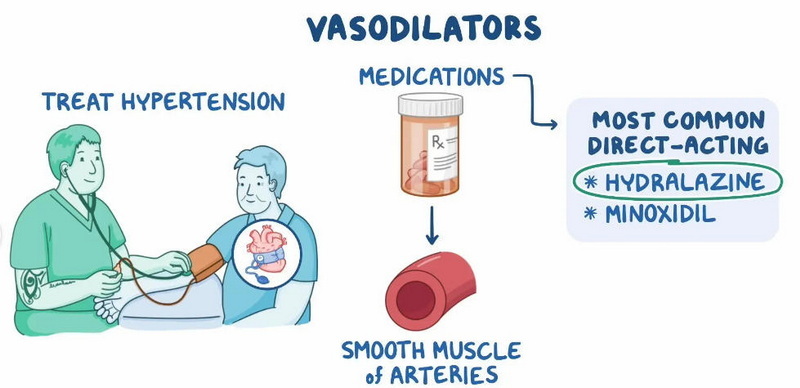
Procaine exerts its anesthetic effect mainly by blocking voltage-gated sodium channels on nerve cell membranes. By inhibiting sodium influx, it halts the initiation and conduction of nerve impulses responsible for sending pain signals to the brain. This sodium channel blockade is primarily why procaine provides localized numbness during procedures.
More than a simple sodium channel blocker, procaine also modulates other cellular processes:
- It interacts with NMDA receptors, reducing excitatory neurotransmission.
- It influences nicotinic acetylcholine receptors involved in signal transmission.
- Its metabolites, particularly para-aminobenzoic acid (PABA), have their own biological activities, including vasodilation and anti-inflammatory effects.
Vasodilation, the process of expanding blood vessels, reduces vascular resistance and enhances tissue blood flow. Procaine's vasodilatory action involves multiple complementary pathways:
- Direct Smooth Muscle Relaxation: Procaine relaxes the vascular smooth muscle cells, causing blood vessels to enlarge.
- Sympathetic Nervous System Inhibition: By blocking sympathetic nerve signals that typically induce vasoconstriction, procaine promotes vessel relaxation.
- Anti-inflammatory Effects: Procaine decreases the release of inflammatory cytokines that contribute to vasoconstriction and tissue swelling.
- Metabolite Actions: PABA, a breakdown product of procaine, enhances vasodilation and acts as an antihistamine, further reducing vessel constriction.
The vasodilatory effects lead to increased regional blood flow, which enhances oxygen and nutrient delivery to tissues. This is particularly beneficial in poorly circulated or inflamed tissues.
1. Enhanced Tissue Healing: Vasodilation improves supply of oxygen and nutrients, accelerating wound healing and repair in conditions with compromised circulation.
2. Pain and Vascular Spasm Relief: Procaine helps alleviate pain due to ischemia and vascular spasms by increasing blood flow in affected areas.
3. Neural Therapy: Intravenous procaine infusions are used to address chronic pain syndromes and circulatory disorders by combining anesthesia, vasodilation, and anti-inflammatory actions.
4. Adjunct in Oncology: Clinical research suggests procaine may reduce side effects of chemotherapy and radiotherapy by improving microcirculation and limiting inflammation.
5. Inflammation Modulation: Through direct and indirect pathways, procaine suppresses inflammatory mediators, which helps in diseases like rheumatoid arthritis.

While vasodilation can improve blood flow, it also accelerates the systemic absorption of procaine from the injection site. This can reduce the duration of localized anesthesia. To counteract this effect, procaine is often administered with vasoconstrictors such as epinephrine, which narrow blood vessels, prolong anesthetic action, and minimize bleeding during procedures.
Procaine is generally safe with a low incidence of allergic reactions compared with other local anesthetics. Side effects related to its vasodilatory properties may include:
- Hypotension: Excessive vasodilation during intravenous administration can lower blood pressure.
- Reflex Tachycardia: The body's response to vasodilation might temporarily increase heart rate.
- Allergic Reactions: Rare, but possible due to procaine or preservatives in formulations.
- Systemic Toxicity: Overdose or intravascular injection can cause central nervous system and cardiovascular toxicity, requiring careful dosage.
Millions of doses administered clinically over decades demonstrate procaine's high therapeutic safety when used appropriately.
Procaine is a local anesthetic with a valuable vasodilator effect that enhances tissue blood flow, supports healing, and contributes to its analgesic and anti-inflammatory properties. This vasodilation results from direct smooth muscle relaxation, inhibition of sympathetic vasoconstriction, and active metabolites. Clinically, these effects improve treatment outcomes in pain management, circulatory disorders, and adjunct oncological therapies.
Proper use of vasoconstrictors alongside procaine ensures prolonged anesthesia and minimal bleeding during procedures. For biotechnology, pharmaceutical manufacturers, and health providers, procaine offers a versatile, effective compound with benefits beyond classic anesthesia.
If your organization seeks reliable procaine supply or professional OEM production services, please contact us for tailored solutions meeting stringent quality standards.
Procaine is widely used as a local anesthetic to block nerve impulses and provide pain relief during minor surgery and dental work.
Procaine induces vasodilation by relaxing vascular smooth muscle and inhibiting sympathetic nerve constriction signals. Its metabolites like para-aminobenzoic acid further enhance vessel widening and decrease inflammation.
Because procaine's vasodilation can shorten anesthesia duration, vasoconstrictors like epinephrine are added to prolong numbness and reduce bleeding at the site of injection.
Yes, systemic vasodilation from procaine infusion can lead to hypotension, especially with high doses or rapid administration.
Procaine has a favorable safety profile with fewer allergic reactions and toxic effects compared to some other anesthetics but requires proper dosing to avoid side effects.
[1](https://www.scivisionpub.com/pdfs/the-procainebaseinfusion-a-review-after-twenty-years-of-use-162.pdf)
[2](https://onlinelibrary.wiley.com/doi/10.1155/2017/9804693)
[3](https://www.ncbi.nlm.nih.gov/books/NBK551556/)
[4](https://cdnsciencepub.com/doi/10.1139/y65-005)
[5](https://www.sciencedirect.com/topics/medicine-and-dentistry/procaine)
[6](https://globalresearchonline.net/ijpsrr/v82-1/03.pdf)
[7](https://www.heraldopenaccess.us/openaccess/the-procaine-base-infusion-20-years-of-experience-of-an-alternative-use-with-several-therapeutical-effects)
[8](https://pmc.ncbi.nlm.nih.gov/articles/PMC3403589/)
Hot tags: Procaine Vasodilator, Procaine Effects, Local Anesthetic Properties, Vasodilation Mechanism, Procaine Uses, Procaine Side Effects, Injectable Anesthetics, Procaine Pharmacology, Vasodilator Agents, Procaine Administration