Content Menu
● Procaine Metabolism: Where and How?
>> Plasma and Liver Metabolism
● Pharmacokinetic Characteristics of Procaine
>> Bioavailability and Administration Routes
● Clinical and Biological Implications of Procaine Metabolism
● Procaine in Pharmaceutical Manufacturing and OEM Services
● Frequently Asked Questions (FAQ)
>> 1. Where is procaine metabolized in the human body?
>> 2. What are the primary metabolites of procaine?
>> 3. How quickly is procaine eliminated from the body?
>> 4. Can genetic factors affect procaine metabolism?
>> 5. Does procaine metabolism influence its anesthetic effectiveness?
Procaine is a well-known local anesthetic commonly used in medical and dental procedures to provide temporary numbness and pain relief. Understanding where and how procaine is metabolized in the body is critical for its safe and effective use, particularly in clinical settings and pharmaceutical manufacturing. This comprehensive article explores the metabolic pathway of procaine, its pharmacokinetics, clinical applications, and important manufacturing insights, especially for businesses seeking OEM services in biotechnology, pharmaceuticals, and medical devices.
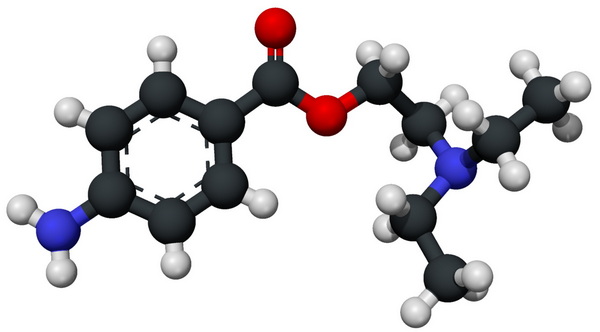
Procaine is an ester-type local anesthetic that acts by blocking nerve impulse transmission through inhibition of sodium ion influx in the neuronal cell membranes. Its primary clinical uses include pain management during dental procedures and minor surgeries. Additionally, procaine is being studied for its potential antioxidant properties and roles in reducing oxidative stress associated with aging and certain chronic conditions, which expands its possible future therapeutic uses.
Procaine is predominantly metabolized in the bloodstream by an enzyme called pseudocholinesterase (also known as butyrylcholinesterase). This enzyme hydrolyzes procaine into two main metabolites:
- Para-aminobenzoic acid (PABA)
- Diethylaminoethanol (DEAE)
This hydrolysis primarily takes place in the plasma but also occurs to some extent in various tissues and organs, including the liver, via microsomal carboxylesterases.
The hydrolysis reaction quickly converts the active procaine molecule into these metabolites, which significantly reduces the anesthetic activity of the compound. PABA is known to be excreted primarily through the kidneys, usually unchanged or conjugated with other compounds, while DEAE undergoes further metabolic degradation and participates in other biochemical processes.
While plasma pseudocholinesterase is the major site of procaine metabolism, the liver plays an important supplementary role, especially in humans and some animal species. In particular, liver enzymes contribute to up to 40% of procaine metabolism in certain animals like cats.
In humans, microsomal enzymes in hepatocytes (liver cells) participate in the detoxification and further metabolism of procaine metabolites. The interplay between plasma and liver enzymatic activity ensures a rapid and effective clearance of procaine and its metabolites from the body.
1. Hydrolysis by pseudocholinesterase breaks procaine into PABA and DEAE.
2. DEAE is further metabolized into ethanolamine.
3. Ethanolamine serves as a building block for membrane phospholipids and is also a precursor to the neurotransmitter acetylcholine, highlighting a potential secondary role of procaine metabolites in neurochemical processes.
Procaine has a notably short plasma half-life of about 7.7 minutes, which means it is rapidly metabolized and cleared from systemic circulation. This rapid clearance explains its relatively short duration of anesthetic effect compared to other local anesthetics such as lidocaine or bupivacaine.
After intravenous administration, steady-state plasma levels are typically reached within 20 to 30 minutes. The distribution half-life (the time taken for the drug to distribute from the bloodstream into tissues) is approximately 2.5 minutes, contributing to its fast onset of action.
The elimination of procaine's metabolites primarily relies on renal excretion, with the kidneys filtering and expelling compounds such as PABA and conjugated metabolites through urine.

Procaine's pharmacokinetics are strongly influenced by its mode of metabolism. Due to rapid hydrolysis by plasma esterases, procaine shows:
- Limited tissue distribution beyond the injection site;
- A short duration of action;
- Rapid elimination through renal pathways.
Its fast metabolism is particularly advantageous in clinical settings requiring short, localized anesthesia without prolonged systemic effects. However, patients with atypical pseudocholinesterase activity may exhibit prolonged anesthetic effects or increased sensitivity to procaine, underscoring the importance of personalized medical evaluation.
Procaine is most commonly administered via infiltration or nerve block injections for localized anesthesia. Oral bioavailability is negligible due to extensive first-pass metabolism in the plasma and liver, meaning oral administration is ineffective for producing local anesthesia.
Intravenous usage is rare but can be employed in specific diagnostic or therapeutic contexts. The rapid metabolism and elimination reduce concerns related to systemic toxicity under normal dosing.
The metabolic breakdown of procaine into PABA and DEAE carries clinical significance beyond simple detoxification.
- Non-toxic metabolites: PABA, once considered a possible allergenic substance, is generally safe at low concentrations resulting from procaine metabolism. It has also been used in ultraviolet protection products for the skin.
- DEAE biological activity: Studies suggest DEAE may possess mild anesthetic effects itself and play roles in biochemical pathways involving neurotransmitter synthesis, indicating potential ancillary effects of procaine beyond nerve blockade.
- Intermediary metabolism: Experimental data point to orally administered procaine hydrochloride influencing cellular metabolism by increasing acetyl coenzyme A ratios and enhancing amino acid incorporation into proteins. These findings hint at possible antioxidant and metabolic modulating properties, which could be relevant in aging research and geriatric medicine, although clinical applications require further validation.
- Drug interactions: Because of the rapid metabolism by pseudocholinesterase, drugs that inhibit or compete with this enzyme can affect procaine's efficacy and duration. Cautious use is advised in patients receiving such medications or having genetic variations in esterase enzymes.
For companies within the biotechnological, pharmaceutical, and medical device sectors, producing procaine that meets stringent quality and safety standards is essential. High-quality manufacturing includes strict adherence to Good Manufacturing Practices (GMP), comprehensive quality control, and reliability in supply.
OEM (Original Equipment Manufacturer) services are widely used by foreign brand owners, wholesalers, and producers seeking customized production of procaine and related products such as benzocaine.
China, as a global manufacturing hub, hosts numerous factories specialized in research, production, and packaging of local anesthetics. These manufacturers offer competitive pricing, precise content control via advanced analytical techniques, and flexible packaging and branding solutions — all critical factors for companies engaged in cross-border sales.
Selecting an experienced OEM partner ensures consistent product performance, regulatory compliance, and the ability to scale up production according to market demand.
Procaine is primarily metabolized in the plasma by the enzyme pseudocholinesterase, with the liver contributing a significant auxiliary role. Its rapid hydrolysis produces mainly para-aminobenzoic acid and diethylaminoethanol, both of which are efficiently excreted from the body. This quick metabolism results in a short half-life and a limited systemic presence, making procaine a fast-acting and generally safe local anesthetic.
Understanding procaine's metabolic pathways and pharmacokinetics is vital for healthcare providers to optimize anesthetic use and anticipate patient-specific responses. For pharmaceutical manufacturers and suppliers, knowledge of these processes ensures effective production and quality assurance for OEM products in both domestic and international markets.
If you are seeking a reliable partner for high-quality procaine manufacturing and OEM services tailored to your business, please contact us. We provide competitive pricing, strict quality control, and customizable options to meet your unique needs and strengthen your brand's position in the global market.

Procaine is mainly metabolized in the blood plasma by the enzyme pseudocholinesterase, with the liver also contributing through microsomal carboxylesterases to a lesser extent.
The main metabolites are para-aminobenzoic acid (PABA) and diethylaminoethanol (DEAE). These compounds are further processed and ultimately eliminated via the kidneys.
Procaine has a short plasma half-life of about 7.7 minutes and is rapidly cleared by renal excretion of its metabolites.
Yes. Variations in pseudocholinesterase enzyme activity due to genetic differences can prolong procaine's effect or increase sensitivity in some patients.
Yes. Metabolites like DEAE exhibit some anesthetic properties, and rapid metabolism limits procaine's duration of action, influencing clinical use and dosing.
[1] https://en.wikipedia.org/wiki/Procaine
[2] https://www.chemicalbook.com/article/procaine-pharmacokinetics-and-clinical-applications.htm
[3] https://go.drugbank.com/drugs/DB00721
[4] https://www.sciencedirect.com/topics/neuroscience/procaine
[5] https://www.made-in-china.com/factory/procaine.html
[6] https://www.chemicalbook.com/ProductDetail_EN_procaine_1804240.htm
[7] https://srcyrl.hnlybiotech.com/active-pharmaceutical-ingredient/benzocaine.html
[8] https://www.ema.europa.eu/en/documents/mrl-report/procaine-summary-report-committee-veterinary-medicinal-products_en.pdf
[9] https://pubmed.ncbi.nlm.nih.gov/3211710/
[10] https://www.pharmacompass.com/manufacturers-suppliers-exporters/benzocaine
[11] https://pubmed.ncbi.nlm.nih.gov/944573/
[12] https://pubmed.ncbi.nlm.nih.gov/1000155/
[13] https://www.bmj.com/content/2/4575/533.2
[14] https://www.sciencedirect.com/science/article/pii/S0022354915427571
[15] https://www.pharmacompass.com/manufacturers-suppliers-exporters/procaine-hydrochloride
[16] https://www.made-in-china.com/factory/benzocaine-cream.html
[17] https://www.sciencedirect.com/science/article/abs/pii/S0021967307002774
[18] https://pubmed.ncbi.nlm.nih.gov/480155/
[19] https://www.veyongpharma.com/procaine-penicillin-g/
[20] https://parchem.com/news/article/parchem-supplies-benzocaine-usp-n000296