Content Menu
● What is Lidocaine HCL and How is it Used?
● Pharmacology and Placental Transfer
● Safety Data and Pregnancy Category
● Use During Different Pregnancy Stages
● Epinephrine Use With Lidocaine in Pregnancy
● Breastfeeding Considerations
● Potential Effects on Fertility and Child Development
● OEM Manufacturing for Lidocaine-Based Products
● Frequently Asked Questions (FAQs)
>> 1. Is Lidocaine HCL safe to use in the first trimester of pregnancy?
>> 2. Can lidocaine creams be safely used while breastfeeding?
>> 3. Does lidocaine increase the risk of birth defects?
>> 4. What are the risks to a newborn if lidocaine is used during delivery?
>> 5. Can lidocaine affect fertility in men or women?
Lidocaine hydrochloride (HCL) is a commonly used local anesthetic, important in many medical, dental, and surgical procedures. For pregnant women, the safety of such drugs is a critical consideration. Understanding whether lidocaine HCL is safe during pregnancy involves reviewing clinical evidence, pharmacology, and expert guidelines. This article provides an in-depth analysis of lidocaine use in pregnancy and breastfeeding, exploring effects on the fetus, dosing considerations, and safety precautions. It also highlights services for international brands seeking custom OEM manufacturing in this medical field.
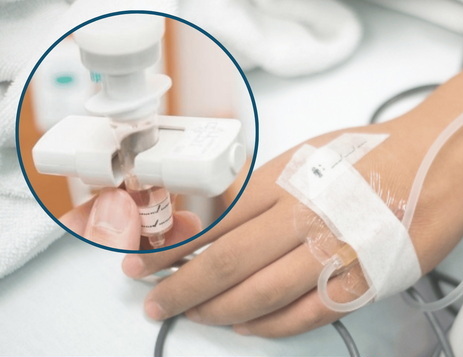
Lidocaine HCL is a local anesthetic that blocks nerve signals in specific body areas to relieve pain. It is available in forms such as injections, topical creams, gels, sprays, patches, and solutions used for epidurals or nerve blocks. In pregnancy, lidocaine is often utilized for:
- Pain management during dental or minor surgery procedures
- Epidural anesthesia for labor and cesarean sections
- Relief of topical pain or skin irritations
Lidocaine is frequently combined with epinephrine to prolong anesthesia and reduce bleeding, though epinephrine use in pregnancy demands cautious consideration.
Lidocaine rapidly crosses the placental barrier through passive diffusion, meaning the fetus can be exposed to the drug following maternal administration. However, the fetus has a limited but existent ability to metabolize lidocaine, and neonatal clearance from the body typically occurs within hours after birth. The extent of fetal exposure depends on the dose, method of administration, and timing relative to delivery.
Lidocaine is classified as a FDA Pregnancy Category B drug, meaning animal studies have not demonstrated risk to the fetus, though well-controlled human studies are limited. Research, including animal reproduction studies at doses significantly higher than human therapeutic levels, have not shown evidence of causing birth defects or fetal harm.
Clinical data from pregnant women also suggest no significant increase in miscarriage risk or birth defects related to lidocaine. Some case reports describe rare neonatal symptoms after maternal anesthesia, like low muscle tone, breathing difficulty, or seizure, but these are uncommon.
- First trimester: Use with caution, as the first trimester is critical for organ development. Though animal studies are reassuring, human data are limited.
- Second and third trimesters: Lidocaine is generally considered safer when clinically indicated. Epidurals with lidocaine are standard during labor.
- Labor and delivery: Lidocaine is widely used for various regional anesthesia techniques. However, toxic effects can occur if dosages are excessive or method of administration is incorrect, affecting mother and newborn.
Epinephrine added to lidocaine prolongs anesthesia and reduces blood loss but constricts blood vessels, including in the uterus. This vasoconstriction may reduce placental blood flow, posing risk in certain conditions such as hypertension or vascular disease in the mother. Therefore, epinephrine use during pregnancy requires careful handling, minimal dosing, and close monitoring.
Pregnant women experience physiological changes that can affect drug metabolism, making careful dose control vital. Typical maximum doses for lidocaine are:
- Up to 4.5 mg/kg without epinephrine (max 300 mg total)
- Up to 7 mg/kg with epinephrine (max 500 mg total)
These limits help prevent maternal and fetal toxicity. Slow administration with aspiration to avoid intravenous injection is recommended. The American Dental Association advises using the lowest effective dose for local anesthesia in pregnancy.
Lidocaine passes into breast milk in very low amounts, and oral absorption by breastfeeding infants is minimal, making it generally safe for nursing mothers. Precautions include washing hands after topical applications and avoiding direct contact of lidocaine cream with nipples. Overall, lidocaine use during breastfeeding presents negligible risk.
There is little evidence that lidocaine affects fertility in either men or women. No studies have linked maternal lidocaine use during pregnancy to behavioral or learning issues in children, though comprehensive research is lacking. Animal studies similarly do not suggest fertility impairment or developmental toxicity.
- Lidocaine is generally safe for use in pregnancy when medically necessary.
- Avoid exceeding recommended doses.
- Use epinephrine cautiously and sparingly.
- Breastfeeding mothers can use lidocaine with minimal risk.
- Consultation with healthcare providers is critical for individual risk assessment.
For international brands, wholesalers, and manufacturers seeking high-quality lidocaine-based pharmaceutical or medical products, our factory offers expert OEM services. We specialize in biotechnology, pharmaceuticals, and medical devices with advanced production facilities, strict quality control, and compliance with international standards. Let us partner with you to produce safe, effective lidocaine formulations tailored to your market needs.
In summary, lidocaine HCL is considered safe for most pregnant and breastfeeding women when used properly and under medical supervision. Animal and limited human data support its non-teratogenic profile, and adverse effects on newborns are rare and typically manageable. Dosage control and cautious epinephrine use remain essential. Patients should always consult healthcare providers before using lidocaine products during pregnancy or lactation. For global brands requiring OEM pharmaceutical manufacturing, our dedicated factory services ensure product quality and compliance, ready to support your business growth. Contact us to know more!
Use of lidocaine during the first trimester is generally considered cautious. Animal studies show no harm, but human data are limited. Always consult a healthcare professional before use.
Yes, lidocaine passes into breast milk in tiny amounts and is poorly absorbed by infants, so it is considered safe. Avoid applying cream directly to the nipple area.
No significant increase in birth defects has been found in studies with lidocaine use during pregnancy.
Rare side effects like low muscle tone or breathing difficulties have been reported but are uncommon and usually treatable.
There is no evidence that lidocaine impacts fertility or increases risks to pregnancies due to paternal exposure.
[1](https://www.ncbi.nlm.nih.gov/books/NBK582791/)
[2](https://www.nhs.uk/medicines/lidocaine-skin-cream/pregnancy-breastfeeding-and-fertility-while-using-lidocaine-skin-cream/)
[3](https://pmc.ncbi.nlm.nih.gov/articles/PMC10315135/)
[4](https://www.nps.org.au/medicine-finder/lignocaine-hcl-injection-bp-single-dose-ampoules)
[5](https://www.accessdata.fda.gov/drugsatfda_docs/label/2010/006488s074lbl.pdf)
[6](https://www.sps.nhs.uk/articles/pain-treatment-during-pregnancy/)
[7](https://bpac.org.nz/2019/otc.aspx)
[8](https://www.medsafe.govt.nz/profs/datasheet/l/lidocaineclarisinj.pdf)
Hot tags: Lidocaine Safety During Pregnancy, Lidocaine HCL Pregnancy Risks, Topical Lidocaine Use Pregnancy, Lidocaine Patch Pregnancy Safety, Local Anesthetic Pregnancy Guidelines, Lidocaine Effects on Fetus, Lidocaine and Breastfeeding Safety, Lidocaine Use in Pregnant Women, FDA Pregnancy Category Lidocaine, Lidocaine Side Effects Pregnancy