Content Menu
● Mechanism of Action: Paracetamol vs. NSAIDs
● Is Paracetamol Officially an NSAID?
● Safety Profile: Paracetamol vs. NSAIDs
● Clinical Uses and Guidelines
● Formulation Challenges for Manufacturers
● Regulatory Perspectives Worldwide
● Market Trends and Opportunities
● FAQ
>> 1. Is paracetamol considered an NSAID?
>> 2. Which is safer for long-term use: paracetamol or NSAIDs?
>> 3. Can paracetamol replace NSAIDs in inflammatory conditions?
>> 4. What are common paracetamol-NSAID combinations?
>> 5. How does your factory support OEM paracetamol production?
Paracetamol, commonly known as acetaminophen, is a cornerstone of pain relief and fever reduction worldwide, but it is not classified as an NSAID. This distinction is essential for healthcare professionals, patients, and manufacturers sourcing active pharmaceutical ingredients (APIs) for global markets.

Paracetamol (acetaminophen) is a synthetic non-opioid analgesic and antipyretic medication widely used to alleviate mild to moderate pain and reduce fever. It is available in various forms including tablets, capsules, oral liquids, suppositories, and intravenous injections, making it suitable for all age groups from infants to the elderly. Chemically, it is N-(4-hydroxyphenyl)acetamide, a para-aminophenol derivative with a molecular formula of C8H9NO2 and a molecular weight of 151.16 g/mol. Paracetamol typically presents as a white, odorless crystalline powder that is sparingly soluble in water but freely soluble in alcohol and acetone.
Its history dates back to the late 19th century when it was first synthesized, but it gained prominence in the mid-20th century as a safer alternative to phenacetin and aspirin for everyday use. Today, it is one of the most consumed over-the-counter (OTC) drugs globally, with billions of doses administered annually. Unlike many painkillers, paracetamol does not cause significant drowsiness or gastrointestinal upset at therapeutic doses, which contributes to its popularity in self-medication scenarios.
In clinical practice, paracetamol is the first-line therapy for conditions like headaches, dental pain, menstrual cramps, and febrile illnesses. Its rapid absorption from the gastrointestinal tract leads to peak plasma concentrations within 30-60 minutes, providing quick relief. Metabolism primarily occurs in the liver via glucuronidation and sulfation, with a small portion converted to the toxic metabolite NAPQI, which is neutralized by glutathione under normal conditions.
Nonsteroidal anti-inflammatory drugs (NSAIDs) represent a diverse chemical class of medications that reduce pain, fever, and inflammation by inhibiting the enzyme cyclooxygenase (COX), which is involved in prostaglandin synthesis. Prostaglandins are lipid mediators that sensitize pain receptors, promote fever, and drive inflammatory responses. Common NSAIDs include ibuprofen, naproxen, diclofenac, aspirin (at anti-inflammatory doses), indomethacin, and celecoxib, a selective COX-2 inhibitor.
NSAIDs are chemically heterogeneous, lacking a single defining structure, but most share a carboxylic acid or enolic acid functional group that facilitates binding to COX enzymes. They are broadly divided into traditional non-selective inhibitors (affecting both COX-1 and COX-2) and COX-2 selective agents designed to minimize gastrointestinal side effects. COX-1 is constitutively expressed and maintains gastric mucosal integrity, platelet function, and renal blood flow, while COX-2 is inducible in inflamed tissues.
Clinically, NSAIDs excel in managing inflammatory conditions such as osteoarthritis, rheumatoid arthritis, ankylosing spondylitis, gout, tendonitis, bursitis, and postoperative swelling. Their anti-inflammatory potency makes them indispensable in rheumatology and orthopedics. However, long-term use requires monitoring due to risks like peptic ulcers, renal toxicity, hypertension exacerbation, and cardiovascular events such as myocardial infarction and stroke.
The mechanism of paracetamol differs fundamentally from NSAIDs, explaining why it is not grouped with them. Paracetamol primarily acts centrally in the brain and spinal cord, where it inhibits a COX-3 variant or COX-1 splice variant, reducing prostaglandin E2 (PGE2) production in the central nervous system. This central action modulates the hypothalamic temperature set-point for antipyresis and activates descending serotonergic and cannabinoid pathways for analgesia. It has negligible peripheral anti-inflammatory effects because it poorly inhibits COX in inflamed tissues at therapeutic concentrations.
NSAIDs, conversely, potently inhibit COX-1 and COX-2 peripherally at inflammation sites, blocking arachidonic acid conversion to prostaglandins and thromboxanes. This disrupts the inflammatory cascade, reducing redness, swelling, heat, and pain. Non-selective NSAIDs like ibuprofen equally block both isoforms, while COX-2 inhibitors spare COX-1 to preserve gastric protection. Additional mechanisms for some NSAIDs include inhibition of lipoxygenases or modulation of nitric oxide pathways, enhancing their broad-spectrum effects.
These mechanistic differences translate to distinct clinical profiles: paracetamol offers clean pain and fever relief without inflammation control, while NSAIDs provide comprehensive symptom management but with organ-specific risks.
No, paracetamol is not officially classified as an NSAID in major pharmacopeias, regulatory guidelines, or clinical textbooks. The World Health Organization (WHO) lists it separately as an analgesic-antipyretic, distinct from NSAIDs. The British National Formulary (BNF) and U.S. Physicians' Desk Reference (PDR) categorize it outside the NSAID class. This separation stems from its weak anti-inflammatory activity—studies show it reduces inflammation only at suprapharmacological doses or in specific models like dental pain with minor swelling.
Historically, some older texts loosely grouped paracetamol with NSAIDs due to superficial similarities like COX involvement, but modern pharmacology recognizes its central predominance and lack of peripheral potency. Regulatory bodies like the FDA and EMA approve paracetamol for pain and fever without anti-inflammatory claims, reserving those for NSAIDs. This classification impacts labeling, marketing, and substitution policies worldwide.
For manufacturers, this means paracetamol products cannot claim "anti-inflammatory" benefits, affecting positioning in markets segmented by therapeutic intent.
Paracetamol boasts a superior safety profile for short-term use in most patients, with rare adverse effects at doses up to 4g/day in adults. Its primary risk is dose-dependent hepatotoxicity from NAPQI accumulation overwhelming glutathione stores, leading to centrilobular necrosis. Risk factors include chronic alcohol use, malnutrition, fasting, or concomitant inducers like isoniazid. Acute overdose (>10g) is a medical emergency treatable with N-acetylcysteine.
NSAIDs pose multifaceted risks from day one: gastrointestinal complications (dyspepsia, ulcers, bleeding) due to COX-1 inhibition reducing mucosal prostaglandins; renal effects (acute kidney injury, interstitial nephritis) from afferent arteriolar vasoconstriction; and cardiovascular hazards (thrombosis, heart failure) linked to COX-2/COX-1 imbalance favoring prothrombotic states. Elderly patients, those with peptic ulcer history, or on antithrombotics face amplified dangers. COX-2 inhibitors mitigate GI but elevate CV risks.
Head-to-head trials confirm paracetamol's edge in at-risk populations: lower bleeding odds ratios and no platelet inhibition. Combination therapy leverages both but demands vigilance.
Paracetamol serves as first-line monotherapy for acute pain (headaches, dysmenorrhea, sore throat), chronic non-inflammatory pain (osteoarthritis without flares), and fever in children, pregnant women, and the frail elderly. Guidelines from NICE, ACP, and AAP endorse it over NSAIDs for these scenarios. In pediatrics, it dominates due to palatability and safety.
NSAIDs dominate inflammatory arthropathies, acute injuries, cancer pain with inflammation, and postoperative protocols favoring swelling reduction. ESC and ACC guidelines restrict NSAIDs in heart failure or post-MI patients, preferring paracetamol. Multimodal analgesia often pairs paracetamol with weak opioids or low-dose NSAIDs for synergy.
In dentistry, paracetamol suits pulpitis without abscess, while NSAIDs target pericoronitis. Migraine protocols favor paracetamol-NSAID combos.
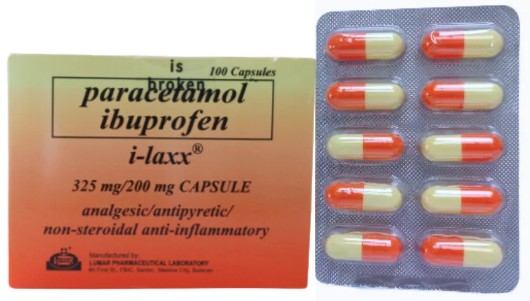
As a leading Chinese OEM factory specializing in biotech, pharma, and medical devices (supplybenzocaine.co.uk), we excel in producing paracetamol APIs and formulations for foreign brands, wholesalers, and producers. Paracetamol's low water solubility (14g/L at 20°C) demands micronization for rapid dissolution in tablets or optimization in effervescents with solubilizers like sodium bicarbonate. Impurities like 4-aminophenol must stay below 50ppm per USP/EP.
NSAID formulations grapple with poor solubility (e.g., diclofenac BCS Class II), gastric irritation (enteric coatings), and polymorphism (naproxen sodium stabilization). We offer sustained-release matrices, fixed-dose combinations (paracetamol-ibuprofen), and sterile injectables compliant with FDA, EMA, and your local regs.
Our cGMP facilities ensure 99.5%+ purity, tailored particle sizes (D50 10-50μm), and stability data for tropical Zone IVb climates. Private labeling, tech transfer, and MOQs from 100kg suit startups to majors.
In the EU, paracetamol is EMA-monographed separately from NSAIDs, with MAHs submitting paracetamol-specific modules. U.S. FDA Orange Book lists acetaminophen distinctly, with OTC monographs excluding anti-inflammatory claims. In Asia, PMDA Japan and NMPA China regulate it as a non-NSAID API.
For exporters, paracetamol enjoys fewer import restrictions than NSAIDs, which face CV risk disclosures in AUS, CAN. We handle DMF filing, CEP procurement, and CTD dossiers for seamless registration.
Global paracetamol demand surges at 4-5% CAGR, driven by OTC growth in emerging markets and combo products. NSAIDs face scrutiny post-ROFECOXIB recall, boosting paracetamol as a safer alternative. Post-COVID, fever/pain segments boom.
OEM partners like us enable brands to launch paracetamol lines affordably, with custom flavors for syrups or vegan capsules. Supply chain resilience from China mitigates shortages.
Paracetamol stands apart from NSAIDs as a centrally acting analgesic and antipyretic with minimal anti-inflammatory action and a hepatotoxicity-focused safety profile, contrasting NSAIDs' peripheral potency and multi-organ risks. This distinction shapes clinical choices, formulations, and market strategies.
Foreign brands, wholesalers, and manufacturers: Partner with our expert Chinese factory (supplybenzocaine.co.uk) for premium paracetamol APIs, finished doses, and NSAID OEM services. From R&D to scale-up, we deliver regulatory-compliant, cost-effective solutions. Contact us today for quotes, samples, and consultations—elevate your product line now! Contact us to get more information!
No, paracetamol is classified as an analgesic and antipyretic, not an NSAID, due to its primarily central mechanism and weak peripheral anti-inflammatory effects.
Paracetamol is generally safer for extended use in patients prone to GI or CV issues, though liver monitoring is essential; NSAIDs require risk mitigation strategies.
Paracetamol cannot fully replace NSAIDs where inflammation predominates, but it complements them or serves as monotherapy for non-inflammatory pain.
Popular combos include paracetamol-ibuprofen for dental/post-op pain and paracetamol-diclofenac for arthritis, offering synergistic relief.
We provide high-purity APIs (>99.5%), custom formulations (tablets, syrups, injectables), packaging, and full regulatory documentation for global markets.
1. https://en.wikipedia.org/wiki/Paracetamol
2. https://pubmed.ncbi.nlm.nih.gov/23719833/
3. https://pmc.ncbi.nlm.nih.gov/articles/PMC5455842/
4. https://pmc.ncbi.nlm.nih.gov/articles/PMC8654482/
5. https://www.tandfonline.com/doi/full/10.1080/23328940.2021.1886392
6. https://pmc.ncbi.nlm.nih.gov/articles/PMC4809680/
7. https://www.nature.com/articles/sj.bdj.2014.554
8. https://pubmed.ncbi.nlm.nih.gov/15662292/
9. https://pmc.ncbi.nlm.nih.gov/articles/PMC3251190/
10. https://www.sciencedirect.com/topics/medicine-and-dentistry/paracetamol
Hot tags: Paracetamol, NSAIDs, Pain Relief, Acetaminophen, Nonsteroidal Anti-Inflammatory Drugs, Analgesics, Fever Reducer, Pain Management, Side Effects, Drug Interactions