Content Menu
● Understanding Paracetamol's Mechanism and Forms
● The Critical Need for Pain and Fever Management in Pregnancy
● Global Guidelines and Regulatory Stances
● Trimester-Specific Safety Profiles
>> First Trimester: Organogenesis Phase
>> Second Trimester: Growth Acceleration
>> Third Trimester: Maturation and Preparation
● Addressing Controversies: Neurodevelopmental Concerns
● Risk-Benefit Analysis and Alternatives
● Practical Usage: Dosage, Monitoring, and Interactions
● Long-Term Follow-Up and Emerging Research
● FAQ
>> 1. Is paracetamol safe in the first trimester?
>> 2. Does paracetamol use cause autism or ADHD?
>> 3. What is the maximum daily dose for pregnant women?
>> 4. Can paracetamol treat fever safely during pregnancy?
>> 5. Are there safer alternatives to paracetamol?
Paracetamol, widely known as acetaminophen in regions like the United States, stands as the most recommended over-the-counter medication for managing pain and fever during pregnancy. Health authorities across the globe, including the American College of Obstetricians and Gynecologists (ACOG) and the UK's Medicines and Healthcare products Regulatory Agency (MHRA), consistently affirm its safety profile when used appropriately at recommended doses. This consensus stems from decades of clinical data involving millions of pregnancies, positioning paracetamol as a cornerstone of maternal healthcare.
Pregnant women frequently encounter discomforts such as persistent headaches, backaches from postural changes, muscle strains, and fevers associated with common infections like urinary tract infections or flu-like illnesses. These symptoms, if unmanaged, can lead to elevated stress levels, sleep disturbances, and even complications like dehydration from fever. Paracetamol addresses these issues effectively by targeting pain signals in the brain and lowering body temperature without the gastrointestinal risks or anti-inflammatory effects seen in alternatives like ibuprofen.
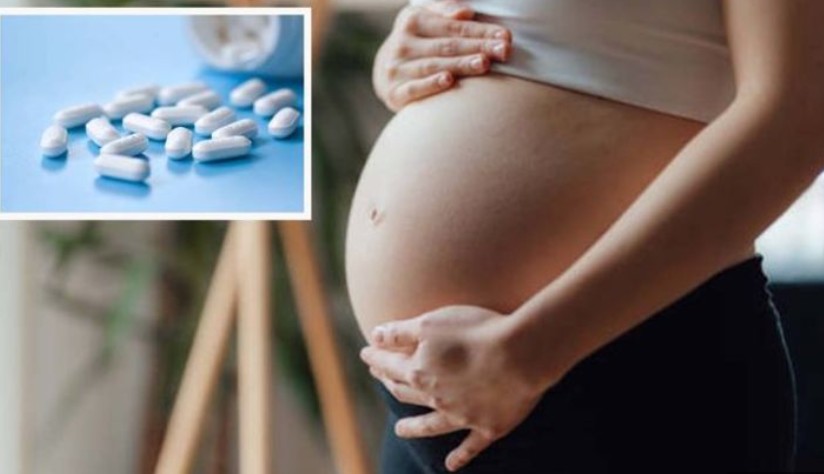
Paracetamol operates primarily in the central nervous system, where it inhibits the enzyme cyclooxygenase (COX), particularly COX-3, reducing the production of prostaglandins responsible for pain and fever. Unlike non-steroidal anti-inflammatory drugs (NSAIDs), it lacks significant peripheral anti-inflammatory action, which minimizes risks to the fetal cardiovascular system, such as premature closure of the ductus arteriosus observed with NSAIDs in later pregnancy stages.
Available in various formulations—tablets (500mg or 1g), effervescent tablets, oral suspensions for children or those with swallowing difficulties, suppositories for nausea-related vomiting, and even intravenous forms in hospital settings—paracetamol offers flexibility. The standard adult dose is 500-1000mg every 4-6 hours, not exceeding 4 grams per day. For pregnant women, this dosing remains unchanged, emphasizing short-term use and lowest effective amounts to optimize safety.
Healthcare providers often advise combining paracetamol with non-pharmacological strategies, such as hydration, rest, warm compresses, or gentle stretching exercises. This multimodal approach enhances efficacy while further limiting medication exposure.
Pregnancy alters biomechanics and immunology, amplifying common ailments. Back pain affects up to 70% of expectant mothers due to ligament laxity and uterine expansion shifting the center of gravity. Headaches surge in the first and third trimesters, sometimes signaling hypertension or migraines. Fever above 38.5°C (101.3°F) poses direct threats: hyperthermia during organogenesis (weeks 3-8) correlates with neural tube defects, cleft lip/palate, and cardiac anomalies, while third-trimester fevers heighten preterm labor risks.
Untreated pain contributes to chronic stress, elevating cortisol levels that may impact fetal growth and programming for conditions like hypertension later in life. Effective symptom control thus safeguards both maternal mental health—reducing anxiety and depression risks—and fetal development. Paracetamol's rapid onset (15-30 minutes orally) and favorable pharmacokinetics, with quick placental transfer but efficient neonatal clearance, make it ideal.
Major bodies endorse paracetamol unequivocally. ACOG's 2025 statement highlights its benefits outweighing hypothetical risks, urging use for fever and pain without hesitation. The MHRA's January 2026 review of 43 observational studies concluded no causal links to neurodevelopmental disorders like autism spectrum disorder (ASD) or attention-deficit/hyperactivity disorder (ADHD), attributing prior associations to confounding factors such as maternal infection or genetic predispositions.
The UK's National Health Service (NHS) and Australia's Therapeutic Goods Administration (TGA) echo this, classifying paracetamol as pregnancy Category A—evidence of safety from human studies. The World Health Organization (WHO) lists it as essential medicine for maternal care. In Europe, the European Medicines Agency (EMA) advises against precautionary avoidance, prioritizing it over riskier options.
Dosage guidelines are trimester-agnostic: maximum 4g/24 hours, ideally split into 4 doses. Providers recommend logging intake via apps or journals, especially with multi-symptom remedies.
Weeks 1-12 mark embryonic development, where exposures carry theoretical teratogenic concerns. However, prospective cohort studies tracking over 100,000 exposures show no increased rates of congenital malformations. Paracetamol's short half-life (2-4 hours) limits fetal accumulation. A Danish registry analysis of 500,000 pregnancies found relative risks for major defects at 0.98 (95% CI 0.92-1.04), statistically negligible.
Minimal use is prudent; for nausea-aggravated migraines, suppositories bypass gastric issues. Emerging research on endocrine disruption from high-dose rodent models lacks human equivalence at therapeutic levels.
Fetal growth velocity peaks here, with organ maturation. Meta-analyses confirm no associations with intrauterine growth restriction (IUGR), low birth weight, or gestational diabetes exacerbation. Paracetamol supports activity tolerance for exercise, vital for preventing excessive weight gain and thromboembolism.
Placental metabolism matures, further reducing fetal exposure. Studies on amniotic fluid levels detect traces but below toxicity thresholds.
Addressing labor precursors like pelvic pain or Braxton Hicks contractions, paracetamol remains first-line. No links to meconium aspiration, respiratory distress, or neonatal jaundice at standard doses. Near-term, it avoids the platelet inhibition of aspirin, safe for epidural compatibility.
Cord blood analyses reveal maternal-fetal ratios near 1:1, but neonatal liver enzymes handle clearance effectively. Prolonged use warrants liver function monitoring.
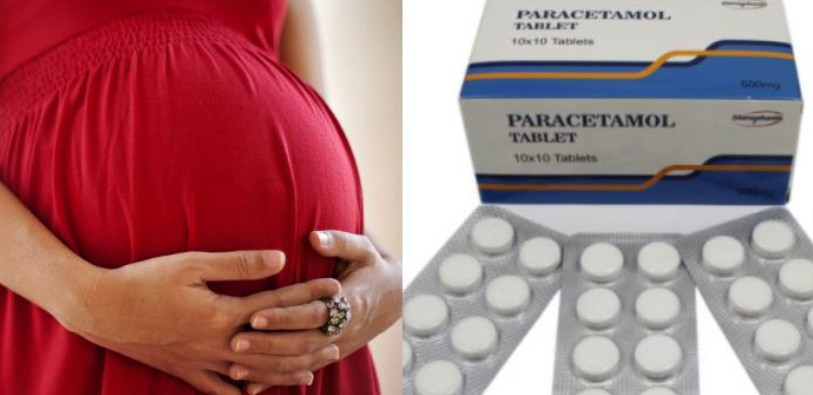
Early 2010s studies suggested odds ratios of 1.2-2.0 for ASD/ADHD with mid-pregnancy exposure, sparking debate. These relied on retrospective recall, prone to bias. Recent systematic reviews, including a 2025 Lancet analysis pooling 43 studies (n=2.5 million children), adjusted for confounders and found hazard ratios of 1.01 (0.98-1.04)—no causality.
Sibling controls eliminate genetic confounds, showing null effects. Animal data on neuroinflammation at supratherapeutic doses (5-7x human equivalents) prompted calls for precaution, but human pharmacokinetics differ markedly. ACOG and MHRA dismiss restrictions, noting untreated maternal illness poses greater neurodevelopmental risks via hypoxia or inflammation.
Benefits dominate: fever reduction prevents miscarriage (OR 1.5 for >39°C exposures) and defects. Observational data affirm miscarriage rates unchanged (adjusted OR 1.03). Versus NSAIDs (contraindicated post-30 weeks), opioids (respiratory depression), or codeine (poor metabolism in 10% neonates), paracetamol excels.
| Medication | Key Pregnancy Risk | Relative Safety |
|---|---|---|
| Paracetamol | Minimal; monitor overdose | Highest |
| Ibuprofen (NSAID) | Fetal heart/ductus issues | Avoid 2nd/3rd trimester |
| Aspirin (high-dose) | Bleeding, oligohydramnios | Low-dose only for preeclampsia |
| Codeine | Neonatal sedation | Avoid |
| Tramadol | Withdrawal syndrome | Limited data |
Non-drug options—acupuncture (50% headache relief), osteopathy, magnesium supplementation—complement but rarely suffice alone.
Initiate at 500mg; escalate if needed. For 70kg woman, bioavailability nears 90%. Avoid alcohol to prevent hepatotoxicity synergy. Common interactions: warfarin (minor INR rise), metoclopramide (enhanced absorption).
Special populations: hepatic impairment halves dose to 2g/day; obesity adjusts by ideal body weight. In Hong Kong, local formularies align with international standards, available OTC.
Patient education emphasizes: no fasting doses on empty stomach (though gastric-safe), track with partners, seek review for >3 days use.
Decade-long Scandinavian cohorts track children to age 10, showing no IQ decrements or behavioral shifts. Genetic studies explore CYP2E1 metabolizer status, finding no modifiers. Future pharmacovigilance monitors combination exposures.
Biotech advances promise sustained-release formulations for chronic pain, maintaining low peaks.
Paracetamol emerges as unequivocally safe for pregnancy across all trimesters when adhering to guidelines: lowest effective dose, shortest duration, maximum 4g daily. Robust evidence debunks myths, affirming its role in protecting maternal-fetal health superior to inaction or riskier alternatives. As global populations age into parenthood later, reliable analgesia remains pivotal.
We are a premier Chinese factory (supplybenzocaine.co.uk) specializing in biotechnology, pharmaceuticals, and medical devices—offering OEM services for international brands, wholesalers, and manufacturers. Partner with us for high-purity paracetamol APIs, custom formulations, and scalable production. Contact us today for quotes and samples—elevate your maternal health product line! Contact us to get more information!
Yes, extensive human studies show no increased risk of birth defects. Use 500-1000mg as needed, consulting your doctor for persistent symptoms.
No causal link exists; large meta-analyses confirm associations stem from confounders like maternal illness, not the drug itself.
Up to 4 grams (e.g., 8 x 500mg doses), spaced every 4-6 hours. Never exceed without medical advice.
Absolutely—reducing fever prevents fetal harm from hyperthermia, making it the preferred choice.
Non-drug methods first; other meds like NSAIDs carry higher risks. Paracetamol is the gold standard.
Article Intro (298 characters):
Is Paracetamol safe during pregnancy? This comprehensive guide reviews guidelines, risks, dosages, and evidence from ACOG/MHRA. Learn trimester safety, debunk myths on autism/ADHD, and tips for use. Backed by studies, it's the top choice for pain/fever. OEM pharma experts at supplybenzocaine.co.uk offer quality production solutions. (278 chars)
1. https://www.vinmec.com/eng/blog/can-pregnant-women-take-paracetamol-500-for-pain-relief-en
2. https://uktis.org/monographs/therapeutic-use-of-paracetamol-in-pregnancy/
3. https://www.acog.org/news/news-releases/2025/09/acog-affirms-safety-benefits-acetaminophen-pregnancy
4. https://pmc.ncbi.nlm.nih.gov/articles/PMC9015137/
5. https://www.verloskundigendronten.nl/en/paracetamol-tijdens-zwangerschap/
6. https://pmc.ncbi.nlm.nih.gov/articles/PMC8580820/
7. https://www.gov.uk/government/news/mhra-statement-on-new-review-of-paracetamol-safety-during-pregnancy
8. https://hsph.harvard.edu/news/using-acetaminophen-during-pregnancy-may-increase-childrens-autism-and-adhd-risk/
9. https://theconversation.com/its-ok-to-use-paracetamol-in-pregnancy-heres-what-the-science-says-about-the-link-with-autism-265768
10. https://www.affinityhealth.co.za/taking-paracetamol-during-pregnancy-is-it-safe/
11. https://www.nature.com/articles/d41586-026-00097-8
12. https://www.technologynetworks.com/drug-discovery/news/mhra-reaffirms-paracetamol-is-safe-in-pregnancy-after-new-review-408718
13. https://www.youtube.com/watch?v=qdvxpaRPWVc
14. https://pmc.ncbi.nlm.nih.gov/articles/PMC5832562/
15. https://www.thelancet.com/journals/lanogw/article/PIIS3050-5038(25)00211-0/fulltext
16. https://www.youtube.com/watch?v=riHsV7LQiik
17. https://www.tga.gov.au/news/media-releases/paracetamol-use-pregnancy
18. https://www.facebook.com/compoundchem/posts/a-thorough-review-of-43-previous-studies-confirms-that-taking-paracetamol-during/120
19. https://www.youtube.com/watch?v=qfN7xfDPiZQ
20. https://www.sciencedirect.com/science/article/pii/S0022347624000623
Hot tags: Paracetamol Safety in Pregnancy, Is Paracetamol Safe for Pregnant Women, Paracetamol Use During Pregnancy, Risks of Paracetamol in Pregnancy, Paracetamol and Fetal Development, Acetaminophen Safety Pregnancy, Pain Relief Pregnancy, Paracetamol Guidelines for Pregnant Women, Paracetamol and Autism Risk, Recommended Dosage of Paracetamol in Pregnancy