Content Menu
● Current Use of Procaine in Dentistry
>> Why Is Procaine Still Relevant?
● The Mechanism of Action of Procaine
>> Pharmacokinetics of Procaine
>> Procaine in Special Populations
● The Future of Procaine in Dentistry
>> Innovations in Dental Anesthesia
● FAQs
>> 1. What is procaine used for in dentistry?
>> 2. Why is lidocaine preferred over procaine?
>> 3. Can procaine cause allergic reactions?
>> 4. Is procaine still available for dental use?
>> 5. What are the side effects of procaine?
Procaine, commonly known by its trade name Novocain, has a long history in the field of dentistry. Introduced in the early 20th century, it was once the go-to local anesthetic for dental procedures. However, with advancements in medical science and the introduction of newer anesthetics, the question arises: Is procaine still used in dentistry today? This article explores the current status of procaine in dental practice, its effectiveness, and its alternatives.
Procaine was synthesized in 1905 by German chemist Alfred Einhorn as a safer alternative to cocaine. It quickly gained popularity due to its effectiveness in blocking pain during dental procedures. Procaine works by inhibiting sodium channels, which prevents nerve signals from transmitting pain sensations. This mechanism made it a valuable tool for dentists, allowing them to perform procedures without causing discomfort to patients.
Procaine was marketed under the name Novocain and became synonymous with dental anesthesia. For decades, it was the standard anesthetic used in dental practices worldwide. However, as the field of dentistry evolved, so did the need for more effective and safer anesthetic options.
Despite its historical significance, procaine is not commonly used in modern dentistry. The introduction of newer local anesthetics, such as lidocaine, has largely overshadowed procaine. Lidocaine offers several advantages over procaine, including:
- Faster Onset of Action: Lidocaine acts more quickly than procaine, providing faster pain relief.
- Longer Duration: Lidocaine typically lasts longer, reducing the need for multiple injections during a procedure.
- Lower Allergic Reactions: Lidocaine has a lower incidence of allergic reactions compared to procaine.
While procaine is not the first choice for most dental procedures, it is still used in specific situations. Some practitioners may opt for procaine due to its unique properties, such as its sympatholytic and anti-inflammatory effects. Additionally, procaine is sometimes used in combination with other anesthetics to enhance their effectiveness.
As mentioned, lidocaine is the most common alternative to procaine in dental practices. Other alternatives include:
- Mepivacaine: Similar to lidocaine, mepivacaine is effective for dental procedures and has a slightly longer duration of action.
- Bupivacaine: Known for its long-lasting effects, bupivacaine is often used for more extensive dental work.
- Articaine: This anesthetic is gaining popularity due to its effectiveness in both infiltration and nerve block techniques.
In many cases, local anesthetics like lidocaine and mepivacaine are combined with epinephrine, a vasoconstrictor. This combination helps to prolong the anesthetic effect and reduce bleeding during procedures. Procaine, being a vasodilator, is often not used with epinephrine, which limits its effectiveness in certain situations.
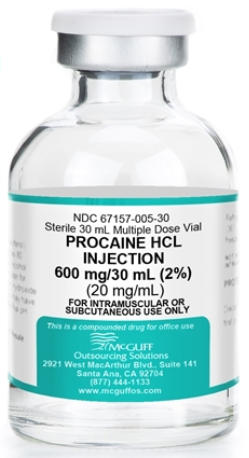
Procaine's effectiveness as a local anesthetic is primarily due to its ability to block sodium channels in nerve cells. When injected into the tissue, procaine diffuses across the nerve membrane and binds to the sodium channels, preventing the influx of sodium ions. This action inhibits the generation and propagation of action potentials, effectively blocking the transmission of pain signals to the brain.
Understanding the pharmacokinetics of procaine is essential for its effective use in dental procedures. Procaine is rapidly metabolized in the body, primarily by plasma cholinesterase enzymes. This rapid metabolism results in a short duration of action, typically lasting about 30 to 60 minutes. The quick breakdown of procaine can be advantageous in certain dental procedures where a short anesthetic effect is desired.
While procaine is generally considered safe, it is not without its risks. Some potential side effects include:
- Allergic Reactions: Although rare, some patients may experience allergic reactions to procaine, which can manifest as skin rashes, itching, or more severe anaphylactic reactions.
- Systemic Toxicity: In rare cases, procaine can lead to systemic toxicity, especially if injected into a blood vessel. Symptoms may include dizziness, tinnitus, and seizures.
- Injection Site Reactions: Patients may experience discomfort, swelling, or bruising at the injection site.
The use of procaine in special populations, such as pregnant women or patients with underlying health conditions, requires careful consideration. Some studies suggest that procaine may be safe for use during pregnancy, but it is essential for practitioners to weigh the benefits against potential risks. Additionally, patients with cardiovascular conditions may require alternative anesthetics due to the vasodilatory effects of procaine.
As dental practices continue to evolve, the role of procaine may further diminish. However, ongoing research into the properties and applications of procaine could lead to renewed interest in its use. For instance, studies exploring the combination of procaine with other agents to enhance its efficacy or reduce side effects may open new avenues for its application in dental anesthesia.
The field of dental anesthesia is constantly advancing, with new techniques and technologies emerging. Innovations such as computer-controlled local anesthetic delivery systems and the use of ultrasound for nerve localization are changing the landscape of dental anesthesia. These advancements may influence the future use of procaine and other local anesthetics in clinical practice.
In conclusion, while procaine played a significant role in the history of dental anesthesia, its use has declined in favor of more effective alternatives like lidocaine and mepivacaine. However, procaine still holds relevance in specific contexts, particularly for practitioners who appreciate its unique properties.
If you are a dental professional or a supplier looking for reliable anesthetic options, consider exploring the various products available, including procaine and its alternatives. For more information or to discuss OEM services for anesthetic products, please contact us today!
Procaine is primarily used as a local anesthetic to block pain during dental procedures, although its use has declined in favor of newer anesthetics.
Lidocaine is preferred due to its faster onset, longer duration, and lower risk of allergic reactions compared to procaine.
Yes, procaine can cause allergic reactions in some patients, although this is less common with newer anesthetics.
Yes, procaine is still available, but it is not commonly used in modern dental practices.
Common side effects of procaine include injection site discomfort, allergic reactions, and in rare cases, systemic toxicity.
Hot tags: Procaine In Dentistry, Novocain Usage Today, Local Anesthetics Comparison, Procaine Side Effects, Dental Anesthesia Options, Is Procaine Effective, Alternatives to Procaine, Procaine History in Dentistry, Modern Dental Anesthetics, Procaine vs Lidocaine